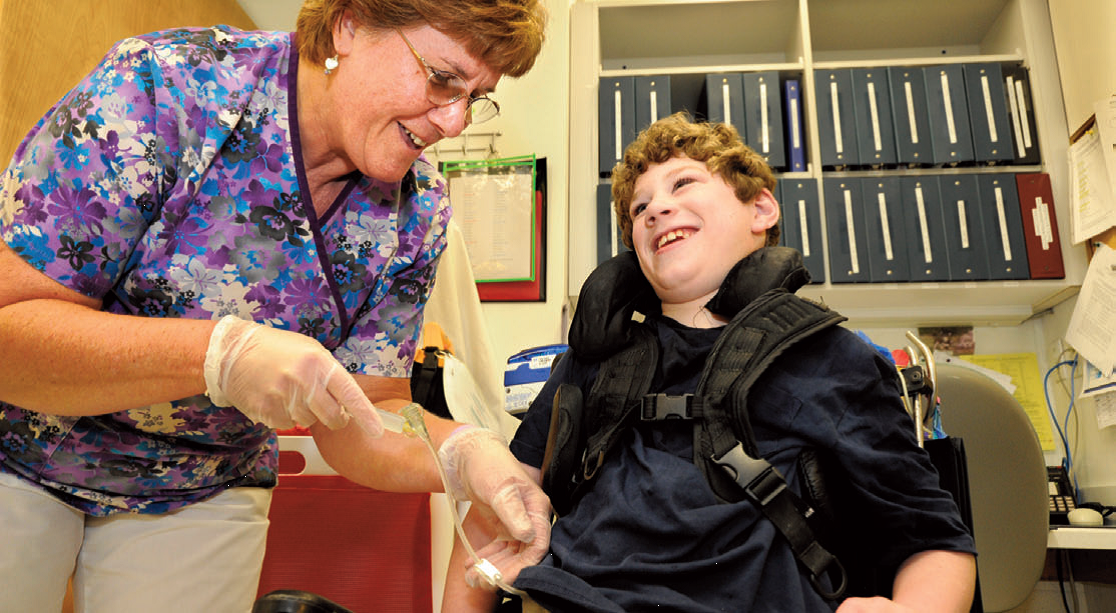
BY RACHEL EZEKIEL-FISHBEIN “Making food appealing, delicious and fun is a way we can ensure our students get their nutritional needs met. Our students are no different than any other students; when you make food fun for them, they’ll want to eat it.”– HMS School
Fourteen-year old Shannon Ward loves to eat, particularly chocolate and, specifically, Nutella, which is what she asked for this Christmas, and Reese’s Peanut Butter Cups. Yet, gaining weight has been difficult for Shannon since she was just over a year, and has been getting more difficult as she’s been going through her adolescent growth spurt. A gastrostomy tube (g-tube) inserted before she was two provides Shannon, who has spastic cerebral palsy, with nutrition and hydration, and helps her meet her nutritional needs for growth. Shannon’s mother, Janine Blythe, is committed to sustaining her daughter’s desire to eat orally. So although eating is not Shannon’s primary source of nutrition, Blythe works closely with HMS School for Children with Cerebral Palsy in Philadelphia, which Shannon has attended since the age of six, to ensure that Shannon eats lunch there with her peers.
At school, Shannon’s g-tube feedings are scheduled so as not to interfere with her daily lunchtime date with her friends. Ask any students—able bodied or disabled—their favorite period of the school day and you’ll find that most favor lunchtime with friends, as Shannon does. Of course, for students like Shannon, with exceptional disabilities, eating lunch often means something very different than wolfing down the typical PB&J. For these students, eating is complicated. Multiple factors enter the equation, such as what textures they can tolerate (Shannon needs her food fork-mashed or pureed with a fork, chopper or blender), appropriate body positioning for eating, oral motor patterns, ability to swallow, motility and elimination problems, ability to thrive, and medical conditions such as reflux that can make eating
challenging and painful and can often dictate food choices. “Eating is labor intensive for Shannon, which means she often burns more calories than she can take in,” explains Blythe. “She has poor oral control. As she’s going through her growth spurt, her tone is increasing and she’s having more difficulty swallowing and eating. She can’t seem to eat the way she’s used to or relax her mouth.” For parents like Blythe, the school can become a powerful adjunct to their child’s medical team, either directly or with the parent as the conduit. HMS’s therapists regularly provide input to students’ physicians. This can include stating concerns, asking questions, pointing out things believed to be impacting a student’s ability to make progress, or offering suggestions that might make things easier for the child.
These insights can alert a physician to the need to change a child’s medicine or formula (for the feeding tube), or revise a child’s nutrition delivery method (an important consideration for children like Shannon, with severe reflux, which is impacted by where the formula goes, the time of day of the feedings, and the speed of the delivery and the volume delivered). Such adjustments can make a huge difference to a child’s comfort and ability to access nutrition. “The medical complexities of our students mean there are a lot of concerns around eating and nutrition,” explains HMS pediatric dietitian Heidi Kecskemethy, RDN, CSP, LDN. “We have a cadre of
specialized therapists and we routinely send information to families and healthcare providers, but any school can contribute to a child’s medical care team.” A common area of concern is growth. At HMS, growth is tracked through thrice yearly height/length and weight checks. Weighing some children requires specialized equipment, like a wheelchair scale. When this is unnecessary, a school nurse can conduct monthly weight checks, saving the family from making frequent
trips to the doctor or a private dietitian.
“It’s very helpful to me to receive regular height and weight updates,” says HMS medical director Steven Bachrach, MD, a pediatric cerebral palsy specialist at Nemours/Alfred I. duPont Hospital for Children in Delaware. “I may only see the child once or twice a year, and it’s very helpful to get this information between visits, so I can make a change in the diet if the child is losing weight or gaining too quickly. Six months or a year is too long to wait to see how they’re responding.” Nutritional tracking and analysis affords important insight into a child’s growth. This starts with logging everything the child eats and drinks, which can be done by the child’s aide or the school nurse. At HMS, a pediatric dietitian analyzes this nutritional data to determine the adequacy of the child’s intake. When there is not a dietitian at the school, the data can be provided to the child’s physician or a private dietitian for analysis.
At HMS, a multi-disciplinary team comprised of Nutrition and Food Service, Speech and Occupational Therapies, Education, and Nursing develops an individualized nutrition plan for each child, based on multiple factors, including growth, need for weight gain or loss, elimination patterns and frequency, food choices and desires, and presence of physical disorders such as reflux. “Through a team approach, we can help discover the root of problems with intake and tolerance, and we can react to concerns raised by healthcare providers. Some people are surprised by who comprises this team. For instance, speech therapists are integral to our work around nutrition,” explains Kecskemethy. Speech pathologists (who can be found at many schools) may focus on a child’s oral motor patterns. Elements of this include:
• What the child is able to physically do with her mouth to manage textures.
• What mobility the tongue has to manipulate food in the mouth.
• The child’s ability to use the tongue to clean the mouth of food.
• The child’s ability to seal her lips so as not to lose food.
• The child’s ability to transport food from the mouth to initiate a safe and effective swallow.
• The child’s ability to move the food from the mouth quickly enough not to risk aspiration.
• The strength and effectiveness of the child’s swallowing.
• The child’s ability to cough and vocalize to clear any materials and pooled secretions.
• The influence of the child’s positioning on their oral motor patterns and GI function.
Pediatric dietitians develop individualized recommendations about the child’s diet (its composition, timing, setting, meals and snacks, etc.), including formula if they have a feeding tube. For students who are not thriving, that means determining how the child can ingest the most calories with least calorie-burning effort. In addition to the specialized jobs of team members, anyone who works with a child has valuable insight to add. “You’re the eyes of the parent and the medical team during the day,” says Anita Rickards, RN, one of HMS’s day student primary nurses, “particularly for students who are nonverbal. Careful observation can tell you if a child is experiencing reflux and in pain, having motility problems, or feeling too full.”
“The observations of people who are watching my patient while she is eating are very helpful to me, particularly when I’m trying to determine whether I need to order a swallowing study,” says Dr. Bachrach, “which has the potential to result in a recommendation to insert a feeding tube.”
According to Dr. Bachrach, a school need not have HMS’s depth of expertise to effectively partner with the healthcare team. He suggests several ways to work with any school:
1. Few schools employ a registered dietitian, but most have a nurse, a physical therapist, an occupational therapist and a speech therapist. Ask your healthcare provider to allow these professionals to access your child’s electronic medical records.
2. If your child sees a developmental pediatrician, email her IEP in advance of your next appointment.
3. Before your child’s IEP meeting, ask your medical team for a letter detailing her needs and supporting necessary therapies.
4. Collaborate with the medical and educational team to ensure that your child can fully participate at school. For instance, plan ahead for school trips and extracurricular activities that include mealtime or snacks, whether this means sending along a blender or chopper, packing a blenderized snack in advance, or chaperoning the trip and mashing your child’s food.
One of the most debated and emotionally charged decisions families confront is whether to insert a feeding tube. The tube acts as a portal, through which food can be delivered directly to the digestive system, so the child is not required to accept all of her nutrition and fluid by mouth. Whether or not to place a feeding tube is a complex decision based upon medical necessity, goals and emotion, and one that is best made with input from the child if they’re able, the medical
team, the parents and the care providers.
Often, families instinctively react negatively to the idea of the feeding tube. Some perceive eating as one of the only ways their child receives pleasure. Others relish mealtime for the chance for positive interaction with their child. Many incorrectly assume that once the child has the feeding tube, she can no longer eat by mouth. “Almost universally, families are very unhappy with the thought of a feeding tube. Nourishment of a child is perceived as a primary function of parenting. To have to give that up can feel like failure,” explains Dr. Bachrach. According to HMS speech pathologist and clinical feeding specialist Marianne Gellert-Jones, MA, CCC/SLP, children with neurological impairments can become more likely to need the help of a tube for supplemental feeding during adolescence. “We can see a student come back to school after summer vacation and look totally different, because they’ve grown several inches or their positioning needs have changed.”
As children grow, their necks elongate and the swallowing structures stretch out. This can make it more labor intensive and difficult for the child to swallow safely, which can increase the challenge of meeting the child’s caloric and fluid needs orally. Often, as the child grows, their demand for calories and fluid increases. These changes in their body and swallowing structures often lead to increased concerns about aspiration. “Physical changes due to growth can be really challenging and disheartening if they adversely influence positioning and safe oral feeding,” says Gellert-Jones, “A student who was a good eater can suddenly find themselves in a situation where they can no longer fully support their nutritional needs by mouth. We may discover that
through physical changes they have become unsafe or unable to completely accept their nutrition orally and thus may need to have a feeding tube. The child hasn’t done anything, but grow. This is the time when our team approach and our relationship with the child’s medical team is crucial. We can pull together therapeutic services and their medical team to brainstorm ways to maintain the child’s positioning and structural integrity, but our best efforts are often not successful when challenged by the child’s ever changing body.” For a family that has resisted placement of a feeding tube, there is often comfort in knowing that every intervention has been attempted. That was the case for HMS student Sarah Mackenzie* and her family.
From the time Sarah entered HMS at the age of eight, her team monitored her growth through height and weight checks. By the end of Sarah’s first year at HMS, the team recognized that Sarah was failing to grow. As a preteen, her ability to eat was lessening, while her nutritional needs for growth for puberty were increasing. Sarah’s physician had been discussing tube placement with the Mackenzies for many years and, like many parents, they were resistant. They were struggling with feelings of failure, because they were unable to provide all of their daughter’s nutrition needs in the typical way. For them, the tube was a physical representation of
everything they could not do for their daughter, and they feared it would stigmatize Sarah. “Every child is individual and a team of experts working with that individual child can help to determine what is feasible for that person,” Kecskemethy reflects. “Dialogue with the parents/care providers is an important part of our job. That entails helping parents to see potential in their child that may have been hidden and to be realistic about challenges and lifelong limitations.”
As Sarah’s medical and therapeutic team worked together unsuccessfully to help her eat orally, her parents gradually recognized that their child’s growth was compromised and came to understand that this was not a failure on their or their daughter’s part. Shortly thereafter, the Mackenzies consented to have a feeding tube placed to provide Sarah with supplemental nutrition. This took a lot of pressure off of Sarah, who began to enjoy eating orally more now
that the stakes were lowered. Ironically, insertion of Sarah’s feeding tube allowed her mealtime
to return to what it is supposed to be—a fun time to enjoy socialization and good tastes.
“Eating is hard for many of our students. We focus on finding the enjoyment in food, from taste to the personal experience of eating with a group of people,” says Doreen Deola, director of food services at HMS. “Making food appealing, delicious and fun is a way we can ensure our students get their nutritional needs met. Our students are no different than any other students; when you make food fun for them, they’ll want to eat it.” As Janine Blythe recognized for Shannon, the importance of socialization while dining can’t be overemphasized, particularly for students for whom communication is difficult. Socializing at meals teaches these students to ask for what they want, communicate discomfort, and interact with peers and caregivers.
Visitors to HMS cannot miss its dining room. The tempting scent of cooking food emanates into the entryway. What transpires in the cafeteria is integral to the school’s programming. Students and staff eat lunch together each weekday, enjoying much the same menu. Pediatric dietitians collaborate with the food services team to develop a menu that is adaptable to the individual needs of each student. “There are various modifications we make, including grounding and pureeing. A huge part of what we do is to make sure the students’ modified food tastes identical to the regular food. If you’re eating a pureed meal, it should taste exactly the same as it does in its original form,” emphasizes Deola. “Taste is everything in eating, so this is critical. It relates to our guiding philosophy of providing our students with as typical a school experience as possible.” With some creativity and guidance, most schools can make mealtime social and enjoyable for children with exceptional needs. Here are some tips:
• If your child can eat orally, ask your child’s school to modify the food the other students eat. Make sure they understand what textures your child can tolerate.
• Work with the school’s food service director to see if favorite foods can be obtained and provided. Send in these foods if the school is unable to provide them.
• Ensure lunch is a social experience by asking that your child be seated with peers, even if the help of a feeder is needed. If your child cannot eat orally, she can still sit and have a social experience with the rest of the students at lunchtime.
• Include nutrition and eating in your child’s IEP.
• If your child needs to gain weight, ask that her diet order include regularly scheduled snacks.•
ABOUT THE AUTHOR:
Rachel Ezekiel-Fishbein is a writer and communications consultant from Elkins Park, PA. She is a mother of three, one of whom has Tourette syndrome, ADHD and anxiety, and is co-founder of the Special Needs Advocacy Group of Cheltenham.
*Name has been changed to protect the privacy of this child.